overview: Autopsy tissue samples from 44 people who died of COVID-19 showed that SAR-CoV-2, the virus that causes coronavirus, spread throughout the body and brain, leaving traces of the virus for up to eight months. rice field.
sauce: University of Minnesota
An analysis of tissue samples obtained from autopsies of 44 people who died of COVID-19 shows that the SAR-CoV-2 virus spread throughout the body, including the brain, and persisted for almost eight months.
This research Nature.
Scientists at the National Institutes of Health (NIH) tested autopsy samples performed between April 2020 and March 2021. They performed extensive sampling of the nervous system, including the brain, in 11 patients.
RNA and surviving viruses in various organs
All patients died of COVID-19 and had not been vaccinated. Plasma from 38 patients was positive for SARS-CoV-2, 3 were negative, and plasma was not available for the remaining 3 of her.
Thirty percent of patients were female, with a median age of 62.5 years. Twenty-seven patients (61.4%) had three or more comorbidities. The median time from onset to death was 18.5 days.
Analysis showed that SARS-CoV-2, as expected, primarily infected and damaged tissues in the respiratory tract and lungs. But researchers also found viral RNA in 84 different body locations and fluids, and in one case isolated the viral RNA 230 days after the patient’s symptoms began.
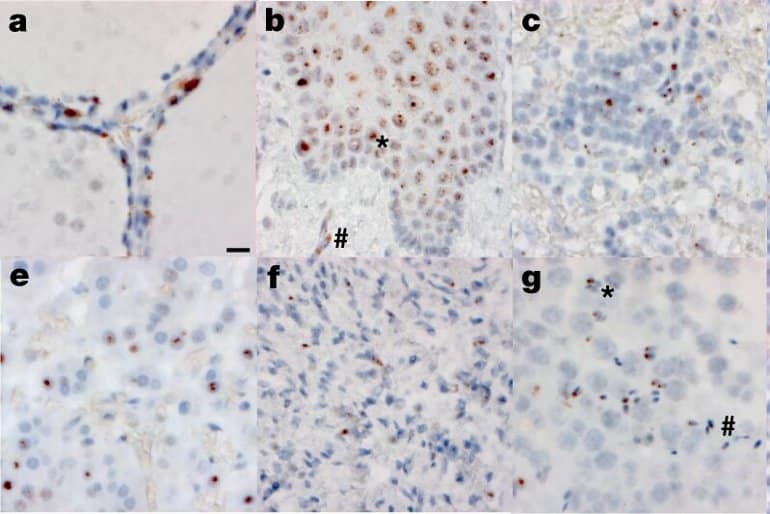
The researchers detected SARS-CoV-2 RNA and protein in the hypothalamus and cerebellum of one patient and the spinal cord and basal ganglia of two other patients. However, little damage to brain tissue was seen, “despite considerable viral load.”
Researchers have also isolated viable SARS-CoV-2 virus from a variety of tissues inside and outside the respiratory tract, including brain, heart, lymph nodes, gastrointestinal tract, adrenal glands, and eyes. They isolated virus from 25 of the 55 samples tested (45%).
“During the first 2 weeks after the onset of symptoms, multiple non-respiratory sites showed viral replication,” the authors wrote.
They add:with high sensitivity [polymerase chain reaction] When [in situ hybridization], isolating viruses in cell culture from multiple non-respiratory tissues, including brain, is a notable difference compared to other studies. “
Potential long-term effects of COVID
Prior to this work, senior study author Daniel Chertow, MD, MPH said in an NIH news release that “in the field, SARS-CoV-2 was thought to be primarily a respiratory virus.” I’m here.
Discovering the presence of the virus throughout the body and sharing that finding with colleagues a year ago led scientists to believe that widespread infected body tissue and the “long COVID”, i.e. weeks to months after infection, We were able to investigate the relationship with subsequent symptoms.
Part of the Paxlovid RECOVER trial, scheduled to begin in 2023, includes: Nature The study is important, according to co-author Stephen Hewitt, M.D., Ph.D., a member of the RECOVER project’s steering committee. Autopsies in the RECOVER trial included people who were vaccinated and infected with the subspecies of concern. This is data that was not available in yesterday’s study.
“We want to replicate data on virus persistence and study its relationship to COVID over time,” said Hewitt. “In less than a year, we have about 85 cases and we are working to scale these efforts.”
About this COVID-19 and Neurology Research News
author: Jim Wapps
sauce: University of Minnesota
contact: Jim Wappes – University of Minnesota
image: Images credited to researchers
Original research: closed access.
“SARS-CoV-2 Infection and Persistence in the Human Body and Brain at Autopsy” by Sidney R. Stein et al. Nature
overview
SARS-CoV-2 Infection and Persistence in the Human Body and Brain at Autopsy
Coronavirus disease 2019 (COVID-19) is known to cause multiple organ failure during acute infection with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), and some patients may develop SARS – Experiencing long-term symptoms called acute sequelae of CoV. -2.
However, the extra-respiratory infection load and time to viral clearance are not well characterized, especially in the brain.
Here, we performed complete autopsies of 44 patients who died of COVID-19 and extensively sampled the central nervous system of 11 of these patients to determine the distribution, replication, and distribution of SARS-CoV-2. Cell type specificity was mapped and quantified. Human body including brain more than 7 months after onset from acute infection.
SARS-CoV-2 is widely distributed, primarily in patients who have died of severe COVID-19, and viral replication is present in multiple respiratory and non-respiratory tissues, including the brain, early in infection. indicates that In addition, persistent SARS-CoV-2 RNA was detected in multiple anatomical sites, including the entire brain, in one case 230 days after symptom onset.
Despite the widespread distribution of SARS-CoV-2 RNA throughout the body, little evidence of non-airway inflammation or direct viral cell pathology was observed. Our data indicate that SARS-CoV-2 can cause systemic infection and persist in the body for months in some patients.

